Digital Twin Patients: The Future of Predictive Surgery Planning
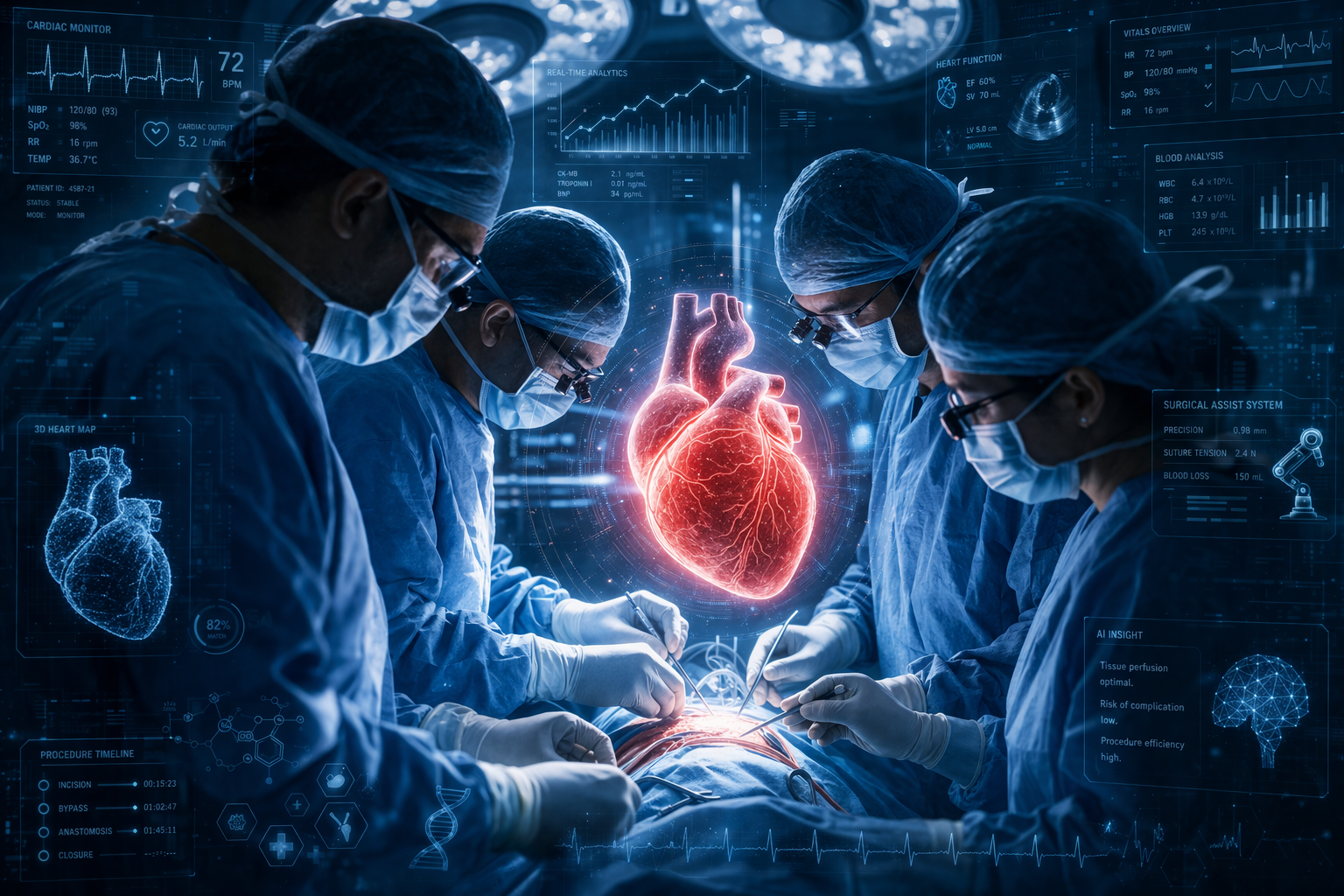
Imagine a world where surgeons can rehearse a complex procedure before ever making an incision—not on a generic simulation, but on a precise digital replica of the patient sitting in front of them. A model that reflects that individual’s anatomy, physiology, and even how their body is likely to respond during surgery. This is the promise of digital twin patients, a rapidly emerging concept that could redefine how surgery is planned, performed, and evaluated.
At its essence, a digital twin in healthcare is a virtual representation of a real patient, built using data from imaging, electronic health records, genomics, wearable devices, and other sources. Unlike static medical images or charts, this model is dynamic. It evolves as new data is added, continuously reflecting the patient’s current condition. For surgical planning, this means clinicians can move beyond estimation and toward simulation.
Traditional surgical planning relies heavily on experience, imaging scans, and clinical judgment. While these methods have led to remarkable advances, they still leave room for uncertainty. Surgeons often need to anticipate how tissues will respond, how blood flow might change, or how a patient’s unique physiology will react under stress. These predictions, while informed, are not always precise.
Digital twins aim to bridge that gap. By integrating multiple layers of patient-specific data into a single computational model, they allow surgeons to simulate different surgical approaches and predict outcomes before entering the operating room. A complex cardiac procedure, for instance, could be modeled to test how altering a valve or rerouting blood flow might affect the patient. Similarly, in orthopedics, surgeons could evaluate how different implant placements would impact mobility and long-term outcomes.
The implications for patient safety are significant. Surgery inherently carries risk, but much of that risk stems from uncertainty. When clinicians can explore multiple scenarios in a virtual environment, they gain a clearer understanding of potential complications and can plan accordingly. This could lead to fewer intraoperative surprises, shorter procedure times, and improved recovery outcomes.
Another major advantage lies in personalization. Healthcare has long aspired to move away from one-size-fits-all approaches, and digital twins bring that vision closer to reality. No two patients are identical, even when diagnosed with the same condition. Factors such as age, genetics, comorbidities, and lifestyle all influence how a patient responds to treatment. Digital twins capture this complexity, enabling care plans tailored to the individual rather than the average.
Beyond the operating room, digital twin technology could transform preoperative discussions with patients. Instead of explaining procedures in abstract terms, clinicians could use visual simulations to show exactly what will happen and why a particular approach is recommended. This level of transparency can improve patient understanding, build trust, and support more informed consent.
Training and education also stand to benefit. Medical students and surgical residents could practice on highly realistic patient-specific models, gaining experience with rare or complex cases that they might not otherwise encounter during training. This could accelerate skill development and improve preparedness for real-world scenarios.
However, the path to widespread adoption is not without challenges. Building an accurate digital twin requires vast amounts of high-quality data, as well as sophisticated algorithms capable of interpreting and integrating that data. Ensuring data interoperability across systems remains a significant hurdle, particularly in healthcare environments where information is often fragmented.
There are also concerns around computational complexity. Simulating biological systems at a high level of detail requires substantial processing power, which may limit accessibility for smaller healthcare organizations. As technology advances, however, these barriers are expected to diminish, much like what has been seen with other data-intensive applications.
Ethical and regulatory considerations add another layer of complexity. Questions around data privacy, ownership, and consent must be addressed, especially when dealing with highly sensitive health information. Additionally, as digital twins begin to influence clinical decision-making, clear guidelines will be needed to define accountability and ensure patient safety.
Despite these challenges, momentum is building. Advances in artificial intelligence, machine learning, and high-performance computing are making digital twin models more feasible and more accurate. At the same time, the growing availability of real-time patient data—from wearables to remote monitoring devices—is enriching the inputs that make these models possible.
Looking ahead, the potential of digital twin patients extends far beyond surgery. These models could be used to predict disease progression, optimize treatment plans, and even test the effectiveness of new drugs in a virtual environment before they are administered. In this sense, digital twins are not just a tool for planning—they are a platform for reimagining how care is delivered.
For now, their most immediate and tangible impact may be in the surgical domain, where precision and preparation are paramount. By enabling surgeons to “practice before performing,” digital twins represent a shift from reactive to predictive care—a shift that could redefine outcomes for both patients and providers.
The future of surgery is not just about better tools or more advanced techniques. It is about better foresight. And in that future, digital twin patients may become one of the most powerful tools clinicians have—offering a window into what lies ahead before the first incision is ever made.