Personal Health Operating Systems: Managing the Body Like Software

For decades, operating systems have quietly orchestrated the digital lives we live—allocating resources, managing processes, and translating complex instructions into seamless user experiences. Now, a similar paradigm is emerging in healthcare. The idea of a “Personal Health Operating System” (PHOS) envisions the human body as a continuously monitored, intelligently managed system—where data flows in real time, decisions are optimized algorithmically, and interventions are delivered with precision. It is a bold shift from episodic care to continuous health management, and it has the potential to redefine how individuals interact with their own biology.
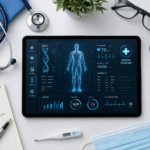
At its foundation, a Personal Health Operating System is a unifying layer that integrates data, analytics, and action. Today’s health data is fragmented across wearables, electronic health records, mobile apps, and clinical systems. A PHOS consolidates these streams into a single, coherent interface, much like an operating system integrates hardware and software components. It ingests biometric signals—heart rate, sleep patterns, glucose levels, activity metrics—and combines them with clinical history, genetic data, and environmental inputs. The result is a living, dynamic profile of an individual’s health state.
What makes this model transformative is not just data aggregation, but orchestration. A PHOS does not simply display information; it interprets it, prioritizes it, and acts on it. Artificial intelligence plays a central role here, analyzing patterns, predicting risks, and recommending interventions. For example, if a user’s sleep quality declines over several days while stress indicators rise, the system might suggest behavioral adjustments, adjust workout intensity, or even prompt a telehealth consultation. In this sense, the PHOS functions as a continuous feedback loop—monitoring, learning, and optimizing over time.
This approach fundamentally changes the relationship between individuals and healthcare systems. Traditionally, healthcare is reactive: patients seek care when symptoms appear, and clinicians respond with diagnosis and treatment. A Personal Health Operating System flips this model by emphasizing prevention and early intervention. It enables individuals to manage their health proactively, guided by data-driven insights. The body becomes less of a mystery and more of a system that can be understood, tuned, and optimized.
From a user experience perspective, the PHOS introduces a new level of personalization. Just as operating systems adapt to user preferences, a health operating system tailors recommendations to an individual’s unique biology, lifestyle, and goals. Two people with the same condition may receive entirely different guidance based on their data profiles. This level of customization is particularly valuable in managing chronic diseases, where standardized treatment plans often fall short. By continuously adapting to real-world conditions, a PHOS can improve adherence, outcomes, and overall quality of life.
The implications for healthcare providers are equally significant. A Personal Health Operating System can serve as a bridge between patients and clinicians, providing a continuous stream of validated data that informs decision-making. Instead of relying solely on periodic visits and limited snapshots of patient health, clinicians gain access to longitudinal insights that reveal trends and patterns. This enhances diagnostic accuracy and enables more precise interventions. It also allows providers to shift from episodic care delivery to ongoing care management, supported by digital infrastructure.
On the business side, PHOS represents a new platform economy in healthcare. Technology companies, insurers, and providers are all vying to become the central orchestrator of health data and services. Revenue models may include subscription-based health platforms, integrated care packages, or value-based contracts tied to outcomes. The entity that controls the operating system layer effectively controls the interface through which health services are delivered, creating significant strategic advantage.
However, building a Personal Health Operating System is not without challenges. Interoperability remains a major hurdle, as data must be integrated from diverse sources that often use incompatible standards. Ensuring data accuracy and reliability is also critical, as decisions based on flawed data can have serious consequences. Robust validation and governance frameworks are essential to maintain trust and safety.
Privacy and security are perhaps the most pressing concerns. A PHOS would handle highly sensitive personal health information, making it a prime target for cyber threats. Organizations must implement strong encryption, access controls, and transparent data policies to protect users. Equally important is giving individuals control over their data—deciding who can access it, how it is used, and for what purpose.
Ethical considerations also come into play. As algorithms increasingly influence health decisions, questions arise حول accountability, bias, and fairness. If a system recommends a particular intervention, who is responsible for the outcome—the developer, the clinician, or the patient? Ensuring that AI-driven recommendations are explainable and equitable will be critical for widespread adoption.
Despite these challenges, the trajectory toward Personal Health Operating Systems is clear. Advances in wearable technology, sensor miniaturization, and AI are rapidly expanding the scope of what can be monitored and managed. At the same time, consumer expectations are evolving, driven by experiences in other digital domains. People increasingly expect their health tools to be as intuitive, responsive, and personalized as their smartphones.
Looking ahead, the PHOS could become the central hub of an individual’s health ecosystem. It might integrate not only medical data, but also nutrition, fitness, mental health, and environmental factors. It could coordinate care across multiple providers, manage insurance interactions, and even interface with smart home systems to create health-optimized living environments. In this vision, health management becomes a continuous, integrated experience rather than a series of disconnected events.
Ultimately, the concept of managing the body like software is about empowerment. It gives individuals the tools to understand and influence their health in ways that were previously impossible. It also challenges healthcare systems to rethink their role—from being the primary source of care to becoming partners in a broader, data-driven ecosystem.
As this paradigm evolves, the success of Personal Health Operating Systems will depend on their ability to balance innovation with responsibility. They must deliver meaningful insights without overwhelming users, protect privacy while enabling data-driven care, and enhance human decision-making rather than replace it. If these challenges can be met, the PHOS could become one of the most transformative developments in the future of healthcare—turning the management of health into a continuous, intelligent, and deeply personalized process.